Areas of Research
Environmental Air Pollution and Cardiometabolic Disorders
Recent reports suggest that in addition to diet and physical activity, urbanization, accompanied by migration to more polluted areas and a 24 h lifestyle could be significant factors fueling the world-wide increase in T2D.
In this context we found that exposure of mice to concentrated PM2.5 (CAP) exacerbates diet-induced systemic insulin resistance and induces early, diet-independent vascular insulin resistance and inflammation. Our work also suggests that the vascular effects of PM2.5 are mediated, at least in part, by pulmonary oxidative stress.
The goal of our current work is to understand the mechanism by which PM2.5 deposition in the lung, the primary target of PM2.5, spreads to cardiovascular tissues and affects cardiovascular and metabolic function and to test whether PM2.5 exposure accelerates the progression to systemic insulin resistance in the susceptible state of dyssynchrony.
For this, we utilize our inhalation exposure system (Versatile Aerosol Concentration Enrichment System, VACES) that simulates real world PM2.5 exposures and mouse models of circadian dyssynchrony.
Identifying the mechanism by which PM2.5 induces vascular and cardiometabolic injury could help to develop strategies to prevent and intervene vascular and cardiometabolic harm due to PM2.5 exposure.
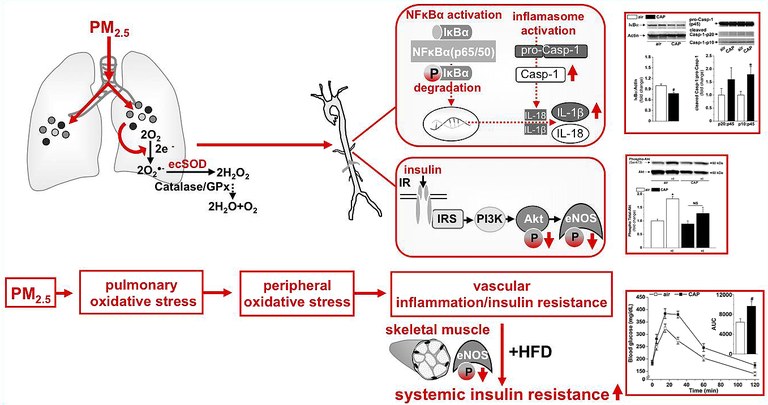
- Haberzettl P, O'Toole TE, Bhatnagar A, Conklin DJ. Exposure to Fine Particulate Air Pollution Causes Vascular Insulin Resistance by Inducing Pulmonary Oxidative Stress. Environ Health Perspect. 2016 Dec;124(12):1830-1839.
- Haberzettl P, McCracken JP, Bhatnagar A, Conklin DJ. Insulin sensitizers prevent fine particulate matter-induced vascular insulin resistance and changes in endothelial progenitor cell homeostasis. Am J Physiol Heart Circ Physiol. 2016 Jun 1;310(11):H1423-38. doi: 10.1152/ajpheart.00369.2015.
Environmental Air Pollution, Diet-induced Obesity and Endothelial Progenitor Cells
Chronic suppression of circulating endothelial progenitor cells (EPCs) is indicative of endothelial injury, and predictive of CVD mortality.
We found that in young, healthy individuals exposure to elevated levels of PM2.5 suppresses circulating EPCs. In mice, we demonstrated that short-term inhalation of concentrated PM2.5 (CAP) decreases circulating EPCs by impairing their VEGF-mediated mobilization from the bone marrow and that improving insulin sensitivity restored EPC homeostasis. Similarly, feeding a high fat diet decreased circulating EPCs while increasing their levels in the bone marrow.
The goal of our current research is to determine the mechanism by which PM2.5 exposure or diet-induced obesity impairs EPC mobilization and function.
Using flow cytometry approaches and cell culture techniques we examine changes in EPC number and function and test for their capability to promote tissue repair in an in vivo model (hind limb ischemia) of vascular injury.
Gaining a better basic understanding of how PM2.5 exposure or diet-induced obesity cause vascular injury could help to identify novel approaches to attenuate CVD mortality and morbidity.
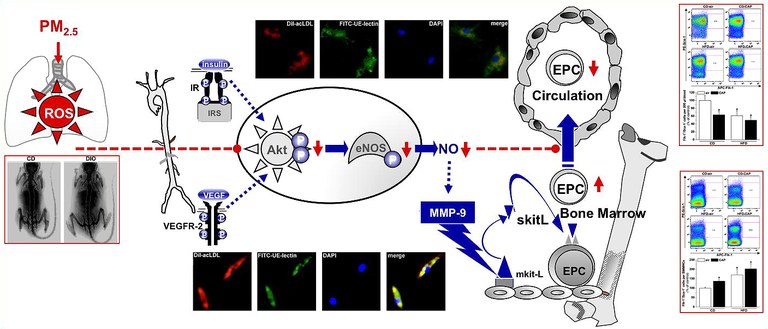
- Haberzettl P, McCracken JP, Bhatnagar A, Conklin DJ. Insulin sensitizers prevent fine particulate matter-induced vascular insulin resistance and changes in endothelial progenitor cell homeostasis. Am J Physiol Heart Circ Physiol. 2016 Jun 1;310(11):H1423-38.
- Haberzettl P, Lee J, Duggineni D, McCracken J, Bolanowski D, O'Toole TE, Bhatnagar A, Conklin DJ. Exposure to ambient air fine particulate matter prevents VEGF-induced mobilization of endothelial progenitor cells from the bone marrow. Environ Health Perspect. 2012 Jun;120(6):848-56.
