SPHIS Home » Departments » Frazier Polypharmacy Program » Prescriptions per Capita
Prescriptions per Capita
Below is a graph representing prescriptions per capita reported by the Kaiser Foundation. Kentucky and the Southeast lead the United States in prescription use. The overall trend in the United States and worldwide is towards increasing polypharmacy as an average of 50 new molecular entities are approved by the FDA to enter the market annually and few to none coming off the market.
Scripts per capita Kaiser Foundation
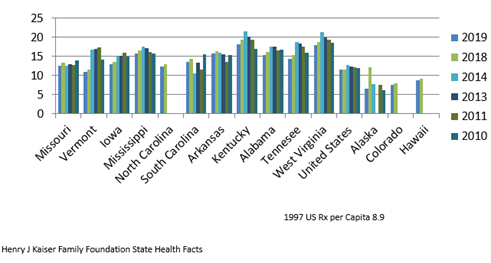
It is fitting that the FPP’s home is here in this region of the United States because the region leads the country in polypharmacy, and the US leads the world in polypharmacy. The level of over-the-counter medications, supplements and products is at an unprecedented high level, with a growing number of products that were once prescription medications.
Beyond the sheer number of products accessible to people there are many more challenges than merely training healthcare providers how to manage polypharmacy. As a society, we need to overcome the risks of random, unchecked polypharmacy which is the at the core of medication harm.
Primary care providers (PCPs) and other providers have the daunting challenge of trying to manage high levels of medications within the confines of the 15-minute office visit.2,3 PCPs are considered the captain of the ship when it comes to overall medication management. People’s medication burden increases with increasing disease burden, increasing number of products on the market both over the counter and prescription, and multiple physicians and providers working in a fragmented system of care. Patient’s medication burden also increases with urgent care visits and hospitalizations. It is difficult for PCPs to be the medication manager, especially because, in addition to the 15-minute office visit, the incentives that drive the way we deliver healthcare don’t allow PCPs the environment to robustly manage medications.
One huge often unanswered question is what goes on in the patient’s medication use “life” outside of the 15-minute office visit? The reality is that 99% of medication management consists of the day-to-day practices in the use of medications, that patients and caregivers implement.
The UofL FPP is working to increase medication literacy among all stakeholders involved. This short video exemplifies a UofL FPP project aimed at helping students gain skills to improve medication literacy in their world and the world around them, now and in the future.
This instructional and inspirational video was created by pre-med student Aysha Khan talks about ways patients (and caregivers) can increase medication literacy: how to use online medication information resources, how to advocate for better medication use communication in the 15-minute office visit, and how to monitor for adverse effects. Aysha created an engaging storyline, and included a common medication class, statins, to demonstrate the type of information patients (and caregivers) need to know to model medication literacy.
Click the video below to watch
Not only did Aysha create a resource to help others, but she will bring her skills forward to her future career as a healthcare professional. The UofL FPP is engaging undergraduate students going toward diverse paths in career choice. Regardless of a student’s future career, polypharmacy will intersect with their work and life. For example, a student may ultimately work in an industrial or legal settings. The impact of polypharmacy on technicians and experts (any workforce member) is an often overlooked but potentially significant factor in the workplace. Thus, the importance of polypharmacy outside of healthcare is increasing as the number of distinct prescription medications continues to grow (there are greater than an estimated 20,000 FDA approved therapeutic agents)
References
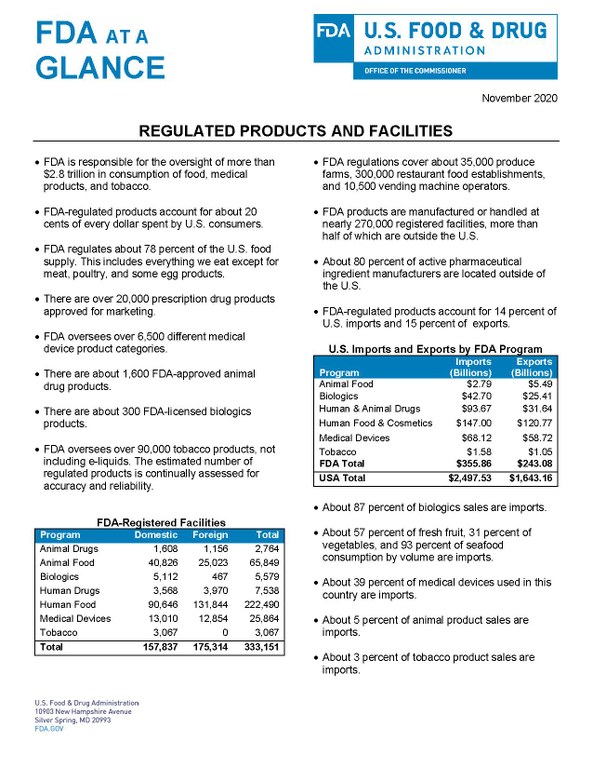
- Kaiser HJF. Henry J Kaiser Family Foundation State Health Facts 2018 found at https://www.kff.org/health-costs/state-indicator/retail-rx-drugs-per-capita/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D. Accessed July 3, 2018. 2018.
- Tai-Seale M, McGuire TG, Zhang W. Time allocation in primary care office visits. Health Serv Res. 2007;42(5):1871-1894.
- Tai-Seale M, McGuire T. Time is up: increasing shadow price of time in primary-care office visits. Health Econ. 2012;21(4):457-476.