Teaching Methods
The ULSOM curriculum requires students to work in teams and collaborative groups over time, to teach their colleagues as they discover new concepts together, and to practice giving and receiving feedback in a professional learning environment.
Problem-Based Learning
In the first two years, MD program candidates work in small groups with faculty oversight to develop their self-directed learning skills and deepen their ability to independently solve clinical problems. This Problem-Based Learning (PBL) thread runs throughout the two years of classroom teaching, requiring students to practice and be assessed on their ability to work collaboratively with others and:
- Assess their own learning needs in relationship to a patient’s clinical problem and develop useful questions for further study
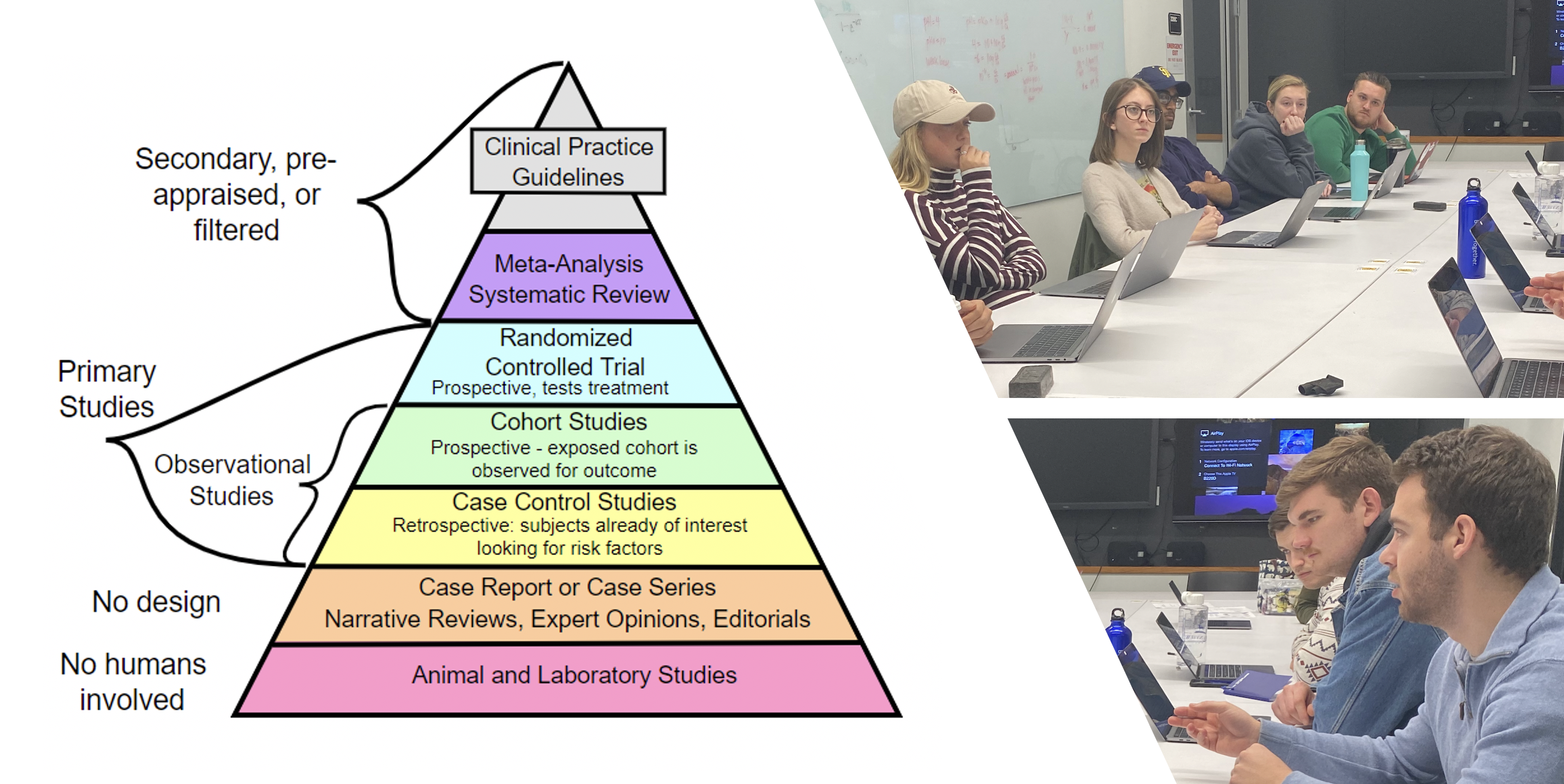
- Research the medical literature to identify, analyze, and synthesize information relevant to solving that clinical problem
- Present their findings, including an appraisal of the credibility and validity of the information they discovered
- Seek and give feedback to their colleagues on their ability to find and apply the information necessary to solve clinical problems
Students are given significant support from the Kornhauser Health Sciences library staff and faculty to support the growth of their self-directed learning skills. Each class in the medical school has a dedicated webpage with curated, research-quality library-owned resources as well as an assigned librarian to support any help needed with informatics or searches. In addition, specifically to support the PBL curriculum, each case has a custom webpage that includes the case, specific resources to assist with that case, and general learning resources appropriate to medical school as well as a specific librarian assigned to assist students in developing their skills. View the PBL library webpage and its associated resources here: https://library.louisville.edu/kornhauser/PBL
Team Based Learning

Team-Based Learning is a specific sequence of active learning tasks that require students to prepare for group learning independently, demonstrate an initial level of knowledge, teach each other to remedy gaps in knowledge, review content with faculty experts, and then apply knowledge further. In TBL, assigned groups of students sit at their table in a large room with all of the other groups in the class to complete these tasks under the supervision of a small number of faculty, differing from PBL which requires separate space and a faculty leader for each small group.
Students prepare for TBL ahead of class by studying materials that are assigned by faculty or have been covered in class that week. When TBL begins, students take a short graded quiz that helps them identify concepts they have mastered and concepts they need help mastering. Next, they work with their small group to take the same quiz as a group to improve their understanding as well as their grade, with peers in the group teaching concepts to each other to improve learning for the whole group. The quiz is then reviewed by teaching faculty and any additional student questions answered. Finally, student groups work through more challenging problems in an open-book format to further apply the concepts covered. TBL and its components are used throughout the first two years of the curriculum, with particular emphasis on weekly TBL’s in the second year of the program.
Other Forms of Active Learning
More than 50% of the ULSOM classroom curriculum is made up of active forms of learning, including online interactive modules, case-based small and large group discussions, and student-led near-peer teaching.
- Softchalk online modules allow faculty to create a customized digital textbook for students that incorporates videos, clinical images, and interactive quizzes and activities. A sample Softchalk module applying concepts in acid-base physiology may be viewed here: https://softchalkcloud.com/lesson/serve/xBQjSJCm7u3k9N/html
- Interdisciplinary Clinical Cases sessions pair a small group of students with the same faculty member for the first two years of the program, meeting monthly to discuss important cases and topics related to medical system function and society. Community advocacy group members also join these groups to help students understand the experience of medical problems and medical care from the patient’s point of view.
- Application exercises place students in small groups for a series of open-book case-based questions that require application of recently learned material and group discussion.
- Near-peer teaching supports the development of students in advanced years of the program as medical school teachers in preparation for residency. Students in their fourth year of medical school can earn elective credit by leading medical student learning experiences under faculty supervision or collaborating with faculty in the creation of durable medical education resources, like a PBL case or TBL session.
The ULSOM is committed to retaining willed body donor dissection as a cornerstone experience in the education of future physicians. Medical students meet their first patient, their assigned anatomical donor, during orientation week and explore the intricacies of Gross and Neuroanatomy in partnership with these patients that have donated their bodies so that students will be better prepared to care for future patients.
Students begin anatomic dissection in the first week of the program and work in the anatomy lab 3 times a week for the fall semester. This work is the ultimate small group patient-centered learning experience, requiring that six medical students work as a team to dissect and practice identifying anatomic structures and their underlying function and relationships. Students are assessed on their ability to create evidence-based presentations of anatomic findings as well as their ability to identify structures on every anatomic donor in the laboratory.
Each spring, students and faculty honor the donors and their families at the Convocation of Thanks, a ceremony that encourages expressions of thanks from students in the form of musical or dance performance, visual art, or written tributes. All students are given the opportunity to reflect on existing art or to create their own art form to honor our donors. These creations are then shared with families at the Convocation to help demonstrate the importance of this experience to their education and formation of professional identity as a physician to the donor’s family. Our educational program and our students are forever indebted to the donors and families that make this program possible.
A link to the Convocation of Thanks webpage can be found here: https://louisville.edu/medicine/departments/anatomy/willedbody/convocation.
More can be found about our Willed Body Program at: https://louisville.edu/medicine/departments/anatomy/willedbody